Living with this condition can be managed

There is a lot of misinformation concerning diabetes, especially when it comes to children and adolescents.
Type 1 diabetes is an autoimmune condition. The body thinks that the cells that create and release insulin are a foreign substance and attacks them. The body becomes insulin deficient because it process sugar improperly. About 60-80% of all pediatric diabetics are Type 1 and symptoms begin showing when they are young.
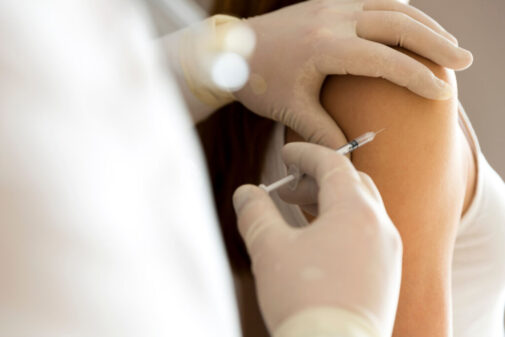
Common symptoms of Type 1 diabetes in children include peeing a lot, drinking a lot of water and losing weight. Unfortunately, the only treatment is insulin, either through a pump or injections. Without insulin, Type 1 diabetes can be life threatening.
However, there are a few different routine tips to keep children and parents from living in fear.
“A big aspect of Type I Diabetes is for the child and parent to be empowered in the process,” shared Dr. Vidhya Viswanathan, a pediatric endocrinologist, with Advocate Children’s Medical Group, “Checking blood sugars frequently helps everyone to learn the blood sugar pattern for that child depending on their carbohydrate count and activity.”
Blood sugars can be checked by doing a fingertip stick or using a wearable glucose monitor, which though a little less accurate can be more convenient. You’ll want to check what your insurance will cover.
Insulin dosing needs to happen every time your child eats. A typical day can entail 4-6 shots a day because insulin is filling the sugar level gap for your body. Based off the carb count and blood sugar levels, there are three ways for your child to receive insulin: from syringes, insulin pens or pumps. Sometimes slightly low blood sugar levels can be treated with fast sugars of around 15 grams like candy, glucose tabs or juice. Then levels can be checked again in 15 minutes to see if that helped.
That can seem like a lot to manage, but Dr. Viswanathan has some tips for how children with diabetes can live normal lives throughout the year.
Get active
Sports are great for diabetes management as it keeps children active and with their friends. Plus, as a family getting outside, enjoying the weather, hiking, etc. should be encouraged.
“Our son plays baseball, flag football, and floor hockey,” says mom Cheri Murray, whose son is a patient of Dr. Viswanathan, “He is good at watching what he eats prior to exercise and adjusting his insulin dose now that he is a teenager.”
Eating Lifestyle
Sometimes when families hear diabetes, they think they will need to change their child’s diet drastically. However, that is not the case.
“I tell my patients to eat better than your neighbors and the standard American diet, but that does not mean eliminating sugars and carbs,” says Dr. Viswanathan, “Good proteins, veggies, fruits, nuts and berries, and things like donuts and cookies have in moderation.”
School Tips
All schools are federally mandated to have someone who can administer insulin to children with diabetes. This also allows children with low sugar levels to eat or leave class to go to the nurse’s office. Together, your child and the school nurse can check their sugar levels and carb intake and give the accurate dosage related to those numbers. Having a flu shot is also beneficial so you and your child do not get the flu. Also, don’t hesitate to have your child notify you, the school counselor, or the school nurse if they are experiencing bullying due to having Diabetes as a common myth can be that it is contagious.
“Every year my husband and I write a letter to all my son’s teachers and coaches about his needs. We also plan a meeting with his teachers prior to school starting,” says Murray. “Our family has also gone to his classroom on the first day of school to speak to his classmates about important signs to watch for when he wasn’t feeling well and how important it is to not share lunches as his carbs need to be counted out. The school nurse was also there and gave an overview of what Diabetes is and this seemed to really help our son and us as parents feel that the school and his friends and classmates were educated and there for our son.”
Related Posts
Comments
One Comment
About the Author
Jennifer Benson, health enews contributor, is coordinator of public affairs for Advocate Health Care and Aurora Health Care. She has 10+ years of community development and communication experience for non-profits and has a BA in Architecture from Judson University in Elgin, IL. Outside of work, you can find her planning the next adventure near water or rocks, re-organizing spaces, working on her Master’s in Public Health, caring for her senior citizen cat, keeping to healthy moving and eating disciplines and growing green things wherever she can find room.
















I believe the first paragraph, third sentence should read “The body becomes insulin deficient because it processes sugar improperly.